ACEs: When Childhood Experiences Don’t Stay in Childhood
You may have seen the term ACEs and wondered what it actually means.
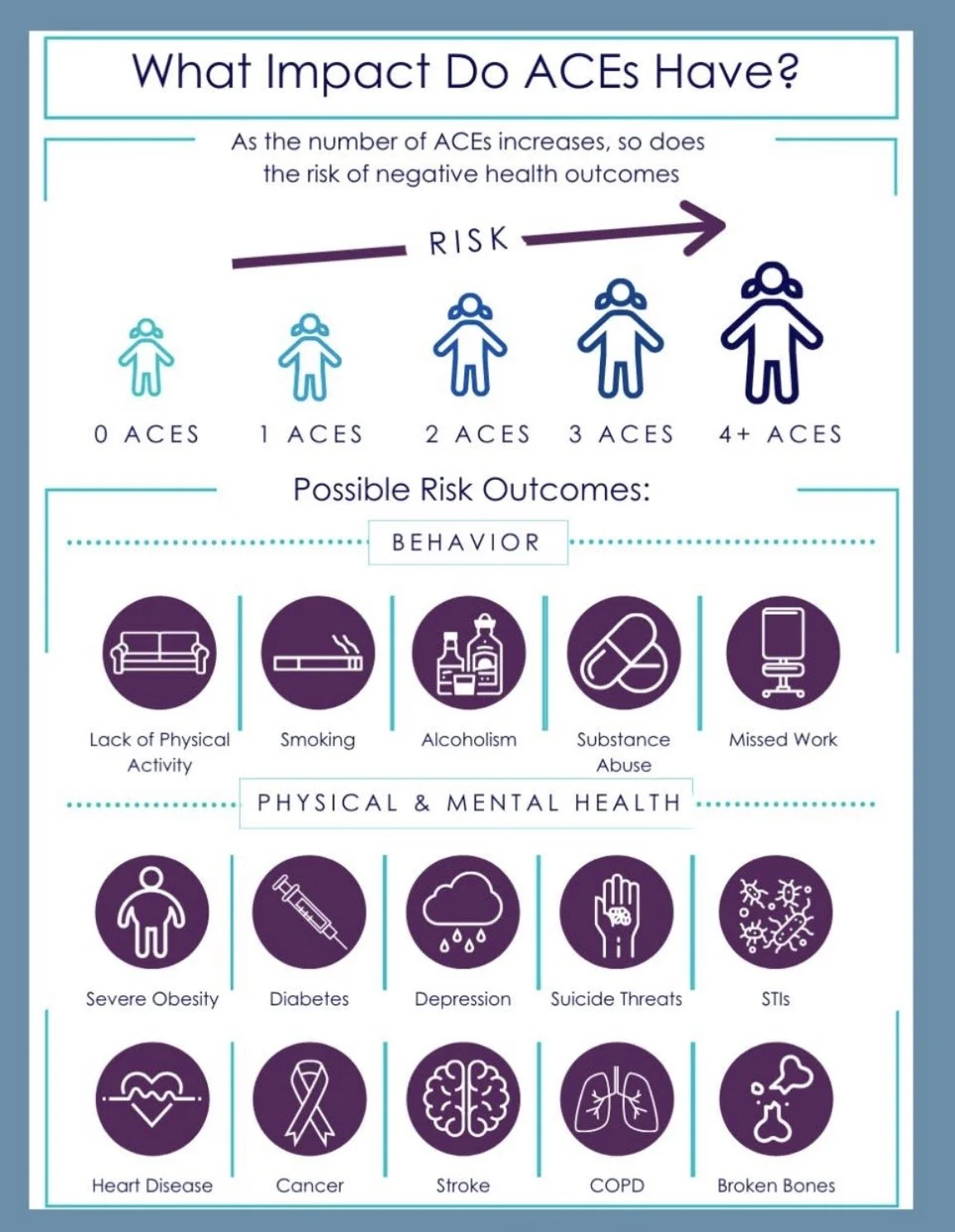
ACEs stands for Adverse Childhood Experiences. The original research looked at difficult or traumatic experiences in childhood, things like abuse, neglect, domestic violence, addiction in the home, parental mental illness, divorce, or loss. What researchers found was powerful: the higher someone’s ACE score, the greater their risk of physical and mental health difficulties later in life.
But here’s the part that matters most to me as a therapist:
Trauma isn’t just what happened.
Trauma is what the brain couldn’t process at the time.
That changes everything.
Because what may not look traumatic to an adult can absolutely be traumatic to a child.
Moving house.
Changing schools.
Parents divorcing.
A parent being emotionally unavailable.
Feeling different.
Being the “sensitive one.”
Not being believed.
Children don’t have adult brains. They don’t have language, perspective, or context. They don’t know, “This isn’t my fault.” They just experience overwhelm.
And when something overwhelms a child’s nervous system without enough support, it becomes an adverse experience.
Children rarely articulate trauma clearly. Instead, it shows up in behaviour.
Clinginess.
Aggression.
Withdrawal.
Perfectionism.
People-pleasing.
Shutting down.
Those behaviours aren’t “bad.” They’re adaptations. They’re survival strategies.
Over time, those strategies can shape attachment, how we connect to others. If safety felt unpredictable, love felt conditional, or emotions weren’t welcomed, we learn to protect ourselves.
That can show up in adulthood as:
• Anxiety that seems to come out of nowhere
• Addiction or numbing behaviours
• Fear of abandonment
• Struggles in relationships
• Feeling “too much” or “not enough”
• Hyper-independence
• Chronic hypervigilance
Sometimes people arrive in therapy saying, “Nothing that bad happened to me, so I don’t know why I’m like this.”
That sentence alone tells me something probably did.
Because trauma isn’t a competition. It’s not about whether it was “bad enough.” It’s about whether your nervous system could cope.
When we experience trauma, the body goes into protection mode. Fight. Flight. Freeze. Flop. Fawn. Those responses are automatic. Involuntary. Designed to keep you alive.
Here’s the important part:
That system doesn’t just switch off because you turned 18.
If a part of you felt unsafe at seven, that seven-year-old nervous system can still get activated at thirty-seven. Your reactions can feel bigger than the current situation because they’re not just about now, they’re about then. The reaction you have is to the 7 year old experience, triggered by something in the here and now.
That’s why you might think afterwards:
“Why did I react like that?”
“I’m so dramatic.”
“That was stupid.”
And then comes shame.
But your body wasn’t being dramatic. It was doing exactly what it was designed to do, detect danger and protect you.
Hypervigilance, always scanning, always on edge, isn’t weakness. It’s a nervous system that learned early that the world wasn’t fully safe.
The exhausting part is carrying that into adulthood when the danger is no longer the same, but the body doesn’t know that yet. Constantly scanning for danger, hyper vigilant and on high alert. Its exhausting, confusing and emotionally painful.
It doesn’t have to stay like this.
This is where counselling can help.
It starts with choosing a therapist you are drawn to and then gel with. Someone you feel gets you. Not every counsellor is for every client, my advice is always chat to a few and explore options.
Once you have chosen, we can start the healing process together.
We don’t always need a detailed memory of what happened. We don’t need to relive everything. Often we start with what’s happening now, the anxiety, the reactions, the patterns.
Through a safe therapeutic relationship, the nervous system begins to experience something new: consistency, attunement, regulation. Slowly, the body learns it’s not alone anymore. And most important pehaps? Feeling safe.
We explore gently. At your pace. Without forcing memories or labels.
Sometimes it’s not about naming the trauma.
It’s about noticing the response.
We work with the part of you that reacts. The part that braces. The part that panics. The part that shuts down.
And instead of shaming it, we understand it.
When you realise, “This reaction makes sense,” something shifts. Compassion grows. The grip of shame loosens.
Your body isn’t broken.
Your reactions aren’t stupid.
Your defence mechanisms aren’t flaws.
They are intelligent responses from a younger version of you who did the best they could. The reactions are involuntary. The bodies way of screaming “warning warning, this is not ok”
Healing isn’t about erasing the past. It’s about helping your nervous system update its information. The trauma memory can shift to the regular memory part of the brain and therefore no need for such strong uncontrollable reactions. The body begins to feel safe rather than on constant high alert.
You are not that powerless child anymore.
But your body may still think you are.
Therapy helps those parts catch up.
And when they do, life can feel lighter, not because nothing hard ever happened, but because you’re no longer fighting yourself for having survived it.
Stay safe. Stay connected. Take gentle care,
Louise x
If this resonates, you’re not on your own.
Pull up a chair.
I've got you.
If you’re tired of carrying it alone, I’m here.
We can take it at your pace. No pressure. No fixing. Just space to be human.
📧 louisemalyancounselling@gmail.com
🌐 www.wildfirecounsellingtherapy.co.uk
Free, no-obligation intro chat, just to see if we’re the right fit.